
Sonographer Reveals What Actually Happens At The 12-Week Baby Scan
Share

There are lots of things we’re told about pregnancy, but when it actually happens to you, you realise there’s so much more to learn. In Unexpected, we’ll chart some of the less spoken about things that happen in the months between finding out you’re pregnant and giving birth.
The 12-week scan is arguably one of the most exciting and nerve-wracking parts of early pregnancy. You get to see your baby for the first time (unless you’ve had an earlier scan) and will finally get to see their tiny heart moving on the big screen.
Many of us think of this scan as the chance to see our baby IRL which can mean we don’t consider the bigger picture of what the scan is actually for. It can also be hard to know how to prepare for the scan. Are you meant to take anything? What do you wear? How long does it last for?
We asked Gill Harrison, professional officer for ultrasound at the Society of Radiographers who has been scanning babies for over 30 years, to walk us through the process and share some things you might not already know.
1. The scan doesn’t always happen bang on 12 weeks
It might be called the 12-week scan, but the dating scan can actually take place anywhere between 10 and 14 weeks of pregnancy. So don’t be disheartened if you get to 12 weeks and still haven’t had yours. You only have to wait a little longer.
2. Don’t wear tight jeans
The day of your scan is nearing, how exciting! Now, choose your wardrobe carefully. “Wear something you’re not worried about getting gel on,” says Harrison, who recommends pairing a skirt or trousers with a top you can easily lift up. If you wear a dress, be prepared to have to lift it right up and lay there in your knickers.
“Don’t wear tight jeans because we’ll probably want you to pull them down further than you can,” she says. “We need to get to the panty line area.”
3. Write down any questions you want to ask ahead of time
You might find that you go to the scan armed with tonnes of questions, but come away with none – or very few – answered.
When you end up lying on that hospital bed, stomach covered in jelly, watching the screen in front of you, it’s not unusual for all the questions you’d safely stored in your brain to disappear into thin air.
All you want to know in that moment is that your baby is OK – and, if they appear to be, watching them dance about on that tiny screen can be the most magical and mesmerising experience. With this in mind, it might be helpful to write your questions down ahead of the scan so you don’t forget them.
That way, once the scanning part is over, you can sit down with your sonographer and ask anything you’ve been meaning to.
And while we’re talking about remembering things, don’t forget your maternity book – most NHS hospitals will issue you with this at your booking appointment. Your sonographer will want to pop your scan results into the book for your midwives to see.
4. Don’t pee beforehand
Sometimes people are asked to attend their scans with a full bladder, as this makes the ultrasound image clearer, so take a bottle of water with you and don’t be tempted to have a wee before you get called into the room. (Easier said than done when pregnant, we know!)
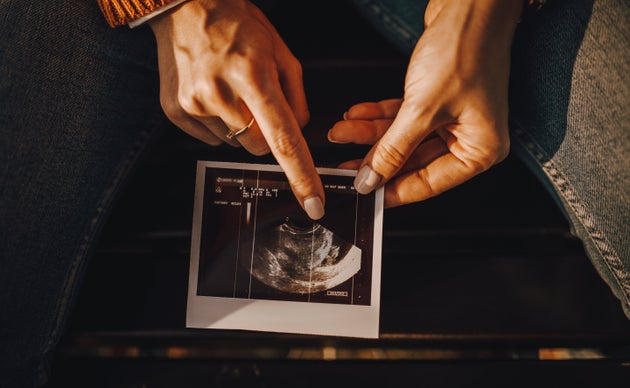
5. It’s so much more than a photo of your baby
Everyone looks forward to the printout you get at the scan which shows you your very own baby in black and white.
But it’s important to bear in mind your sonographer will be looking out for lots of different things during the 20-minute scan, including:
Whether your baby’s heartbeat is present. You should be able to see it pumping on the screen but won’t be able to hear the heartbeat itself.
How many babies there are.
Where the baby is positioned. This is to ensure it’s in the uterus and not outside the uterus (also known as ectopic pregnancy).
To measure their crown to rump length (aka their head to bottom length) to be able to give you a more accurate due date.
Checking some of the structures of the baby to make sure they look normal for that stage of pregnancy.
Screening for Down’s syndrome, Edwards’ syndrome and Patau’s syndrome, if you opted for it. Regardless of whether you opt for it, your sonographer will measure the fluid at the back of the baby’s neck (nuchal translucency) which is linked to these syndromes.
Checking the uterus and ovaries to make sure there aren’t any fibroids or any other masses or cysts.
So yes, lots going on.
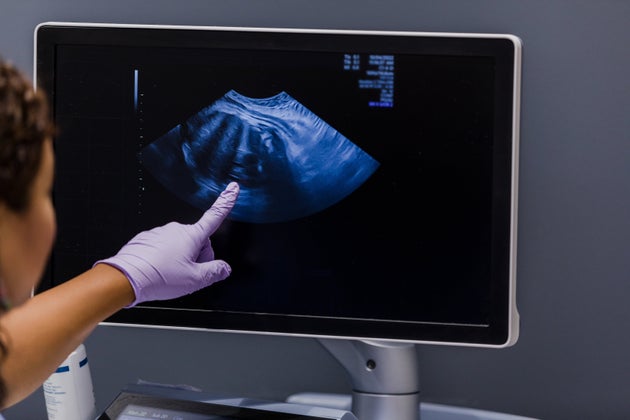
6. It’s not always easy to see everything that’s going on
Sonographers have quite a job on their hands because sometimes, for whatever reason, your tiny baby doesn’t want to play ball. They might be turned away or moving around a lot which can make the sonographer’s job a lot more difficult.
This can mean a lot of moving about with the ultrasound ‘wand’. The sonographer might also have to press down quite hard in order to get a decent picture.
While some sonographers will talk you through what they’re seeing and point things out on the screen, others will be concentrating hard on taking lots of measurements during the scan – so don’t be put out if they’re silent.
Simply ask them to go over their findings once the scanning part has finished – they’ll be more than happy to talk you through the report.
7. Those line graphs on your scan report are ‘centile charts’
When you look over your scan report, you might notice a couple of small charts where a dot is positioned on a scale between two outer lines. “The middle line is what we call the 50th centile,” says Harrison, “so that’s the average.”
This means that if you had 100 babies, all at the same number of weeks, most of them would be on that middle line if there were no complications, says Harrison. But there will always be some that are above and some that are below in the outer lines – because we’re all different.
If the dot appears above (to the right of) the middle line, it’s likely to indicate your baby is a bit bigger than average, and if it’s below (to the left of) the central line it’s likely to be a bit smaller than average.
“It’s trying to work out which of those are normally large or small [babies], and which are those where there’s something wrong with the pregnancy,” says Harrison. So, for example, a baby which is showing bigger on the charts might indicate a diabetic mum, or a baby showing smaller might indicate there’s a problem with the placenta so the baby’s not growing as it should be.
“We need to identify those compared to the normal few who will be big or small because of their genetics,” she explains.
On your report, CRL means crown to rump length, NT refers to nuchal translucency and HC is head circumference.
8. Even if you opt out of screening, the scan may still flag potential issues with your baby
There are two main measurements that are taken at this scan – the length of your baby from head to bottom (to give a more accurate due date), and the nuchal translucency or thickness of fluid at the back of your baby’s back of neck. The latter is used to screen for conditions like Down’s syndrome.
While the screening itself is optional, Harrison points out that if people choose not to have the screening, they might still have things flagged up during the scan that alerts them to possible underlying conditions.
For example, if the measurement at the back of the neck is thicker than 3.5mm there’s a link to cardiac defects, she says. So while the parents might have opted out of screening for the various syndromes, “we would still have to do something and tell them if that measurement was over 3.5mm thick”.
Midwife Louise Broadbridge, also known as The Honest Midwife, says it’s important people are aware of the screening processes that go on throughout pregnancy.
“Everybody really looks forward to that scan at 12 weeks but actually it’s really understanding there is a purpose to it,” she says. “People go very excited for that scan and then can sometimes be told there’s a large nuchal fold or something that needs to be investigated – and they didn’t realise that.”
9. Your sonographer might not be regulated
As you probably know by now, sonographers are the people who carry out your ultrasound scans – however in the UK, ultrasound is not regulated. The issue with this is that if there was some unprofessional behaviour, they could still carry on working, says Harrison.
She suggests people need to be aware of this. “There are people who call themselves sonographers – this is predominantly in some of the private, what we call ‘boutique scanning clinics’ – but they’ve not had any formal training at all. I think that’s the key message for people to be aware of: that sometimes the person doing the scan has very little training.”
That’s not to say all sonographers are in the same boat – many are well qualified and are regulated by other bodies. For example, because lots of sonographers, like Harrison, are qualified radiographers, they are regulated by the Health and Care Professions Council (HCPC).
If you’re concerned about how well trained your sonographer is, you can ask them some questions like: what training have you had? Or, are you registered with a statutory or voluntary register for sonographers? The latter gives some indication there’s been some assessment of their qualifications and references.
10. It’s not always positive news
Sometimes issues can be flagged up at the 12-week scan – some of which require monitoring and others which relate to more serious problems that will undoubtedly be very distressing for those in the room.
Anomalies that can be thrown up include issues with the abdominal wall as well as the bowel, says Harrison. If an anomaly is detected, the parents would be told and would be referred to see a foetal medicine specialist who can offer advice on what the consequences are for the pregnancy and to explore any further problems linked to that. You’ll be offered more scans to double check the anomaly.
In rare cases, a baby’s heart might not be beating or sometimes the baby’s skull doesn’t form at all – sadly there’s not much that can be done about these, which can be very upsetting for the parents.
Harrison says issues with the skull not forming are far less common now than when she first started scanning. “That’s why we recommend folic acid,” she explains. “If people haven’t taken folic acid, particular people who fell pregnant unexpectedly, sometimes the skull doesn’t form at all and there’s absolutely nothing you can do about that. It’s not compatible with life unfortunately.”
If this is the case, parents will be sent for further tests and will be offered support and counselling on what their options are for their pregnancy.
11. You might have to pay for the scan images
If your scan goes well and everything looks as it should, you’ll be offered photo printouts of your baby.
In some hospitals this might be free, however Harrison notes that most of the time you’ll probably have to pay for the pics – so don’t forget to take cash. It shouldn’t cost you any more than a fiver in most NHS hospitals, although some parents have reported having to pay up to £12 for four pics.

Related...
- [TAG4]Pregnancy Sickness Took Over Our Lives. Here's What Got Us Through
- [TAG5]Sonographer Explains How They Actually Tell The Sex Of Your Baby
- [TAG6]I Only Found Out I Was Pregnant At Seven Months
- [TAG7]The Important Life Stage We Should Be Talking About — But You Probably Haven't Heard Of It
- [TAG8]There's A 'Gay Tax' On NHS Fertility Treatment. This Is The Impact
- [TAG9]Ouch. Nurse's Video Shows Why Removing An IUD Isn't Always So Simple
- [TAG10]The Term 'Geriatric Pregnancy' Isn't Just Offensive, It's Also BS